Maine Legislature Considers Ban on Health Care Noncompetes: What Employers Need to Know About L.D. 2200
The Maine Legislature is currently considering proposed legislation that would ban the use of noncompete agreements with state-licensed employees in the health care sector. L.D. 2200, “An Act to Prohibit Noncompete Clauses for Health Care Professionals,” would amend Maine’s noncompete statute to broadly prohibit noncompete agreements for doctors, nurses and many other health care practitioners. What do employers need to know about this proposal and what should you do while we wait for next steps?
Maine’s Existing Noncompete Framework
Maine already regulates noncompete agreements through 26 M.R.S.A. § 599‑A, which outlines the standards for an enforceable noncompete in Maine, but also creates a number of exceptions and protections for employees. Specifically, § 599‑A:
- Bans noncompetes for certain low-wage workers
- Bans noncompetes for veterinarians unless they have ownership in the practice
- Requires employers to disclose that a noncompete will be required prior to issuing a job offer
- Requires employers to provide a copy of a noncompete at least three days before it must be signed
- Delays effectiveness of noncompetes for six months after signing or one year after the start of employment, whichever is later – except for doctors, whose noncompetes do not have such delayed effectiveness.
L.D. 2200 would be a full turnabout for doctors. Rather than having less protection than other employees, they would benefit from a complete ban on health care practitioner noncompetes.
L.D. 2200’s Proposed Ban on Health Care Practitioner Noncompetes
L.D. 2200 would amend § 599-A to completely ban the use of noncompetes with “health care practitioners.” The bill defines “health care practitioner” very broadly to include any individual “qualified or licensed under state law to perform or provide health care services to persons in the State.”
Given this broad definition, this means L.D. 2200 would ban noncompetes not only with doctors, but also with nurses, mental health professionals, and other licensed or “qualified” clinical personnel.
The bill does not elaborate on who may be “qualified” but not “licensed.” For some analogous guidance, however, it may be worthwhile to note that the Maine Health Security Act defines “healthcare practitioner” with some further specificity to include “nurses, podiatrists, optometrists, chiropractors, physical therapists, dentists, psychologists, physician associates and veterinarians.”
Current Status and Forecast for the Bill
L.D. 2200 was reported out of the Joint Standing Committee on Health Coverage, Insurance and Financial Services to implement recommendations from a state commission reviewing health care transaction oversight and service delivery in Maine. The bill reflects the underlying commission’s concern that restrictive covenants may limit patient access to care, particularly in rural areas, and constrain competition in more concentrated provider markets.
The Committee issued a divided report on the bill on February 25, with the majority supporting passage of the bill with amendments, and the minority supporting passage of the bill as written.
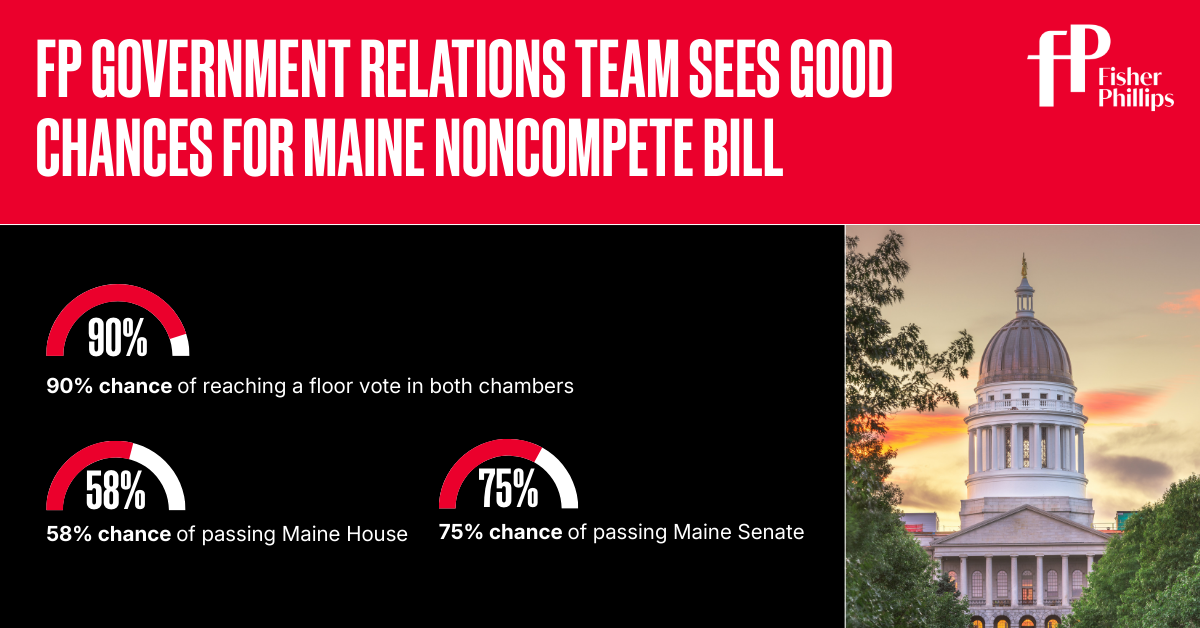
With the divided report issued, our Government Relations Team forecasts that the bill now has a 90% chance to reach a floor vote in both houses of the Legislature. If it hits the floor as expected, our Team forecasts a slightly better than 50% chance of passing the House, but a 75% chance of passing the Senate.
Conclusion
Make sure you are subscribed to Fisher Phillips’ Insights to gather up-to-date information on this and other pending bills. If you have questions, please contact your Fisher Phillips attorney, the authors of this Insight, any attorney in our Portland, Maine, office, or any attorney in our Employee Defection and Trade Secrets Practice Group or our Healthcare Industry Team.